ACQUIRED IMMUNODEFICIENCY SYNDROME (AIDS)
Introduction
AIDS is caused by Human Immunodeficiency Virus (HIV).
- It causes severe suppression of immune system which leads to:
- Opportunistic infections
- Secondary neoplasms
- Neurologic manifestations
- AIDS is diagnosed when the CD4+ T-cell count falls below 200 cells/µL or when AIDS-defining illnesses occur, regardless of CD4 count.
Epidemiology
HIV spreads only when blood containing the virus from an HIV-infected person is injected into another person, or when body fluids containing the virus come into contact with the broken mucosal surfaces of another person.
- Sexual Transmission (Most Common)
- Heterosexual transmission
- Men having sex with men
- Risk Factors:
- High viral load
- Type of sexual activity- Anal sex>Vaginal sex
- Concurrent STDs
- Parenteral Transmission
- Intravenous drug users (due to sharing of contaminated needles and syringes)
- Blood transfusion (Rare now a days due to screening protocols)
- Mother-to-Infant Transmission
- During delivery (Most common)
- Through breast milk
- Prevention:
- Antiviral therapy during pregnancy
- Cesarean section before labor and membrane rupture
- Unknown Factors (~5%)
Etiology
Properties of HIV
- HIV is a Retrovirus (a type of virus that carries its genetic material in the form of RNA instead of DNA.) belonging to Lentivirus Family
- Two Types:
- HIV-1: Most common worldwide (USA, Europe, Africa)
- HIV-2: Mainly in West Africa and India (It generally progresses more slowly and is less transmissible than HIV-1)
Structure of HIV
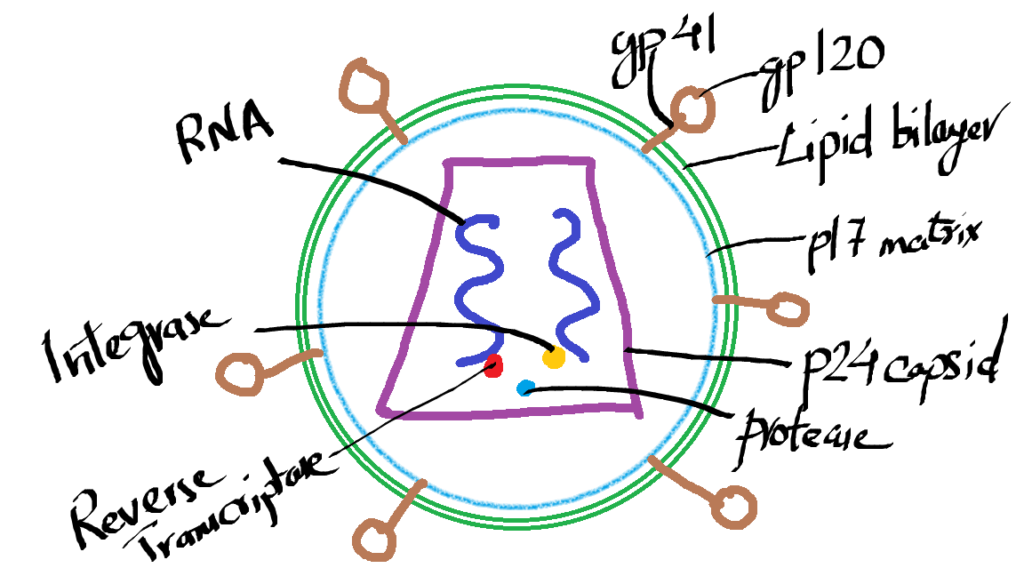
- Spherical Virion with Lipid Envelope
- Core:
- Matrix Protein: p17
- Envelope Glycoproteins:
- gp120 (Attachment to host cells, highly variable)
- gp41 (Fusion with host membrane)
- p24 (Major Capsid Protein) – Used for diagnostic tests
- Enzymes: Reverse Transcriptase, Integrase, Protease
- Two RNA copies
HIV Genome
- gag Gene: Encodes capsid proteins (p24, p7, p9)
- pol Gene: Encodes enzymes (Reverse Transcriptase, Integrase, Protease)
- env Gene: Encodes envelope proteins (gp120, gp41)
- Regulatory Genes: tat, rev, vif, nef, vpr, vpu (Control replication and pathogenicity)
Pathogenesis of HIV Infection and AIDS
- HIV mainly affects cell-mediated immunity due to → loss of CD4+ T cells
Life Cycle of HIV
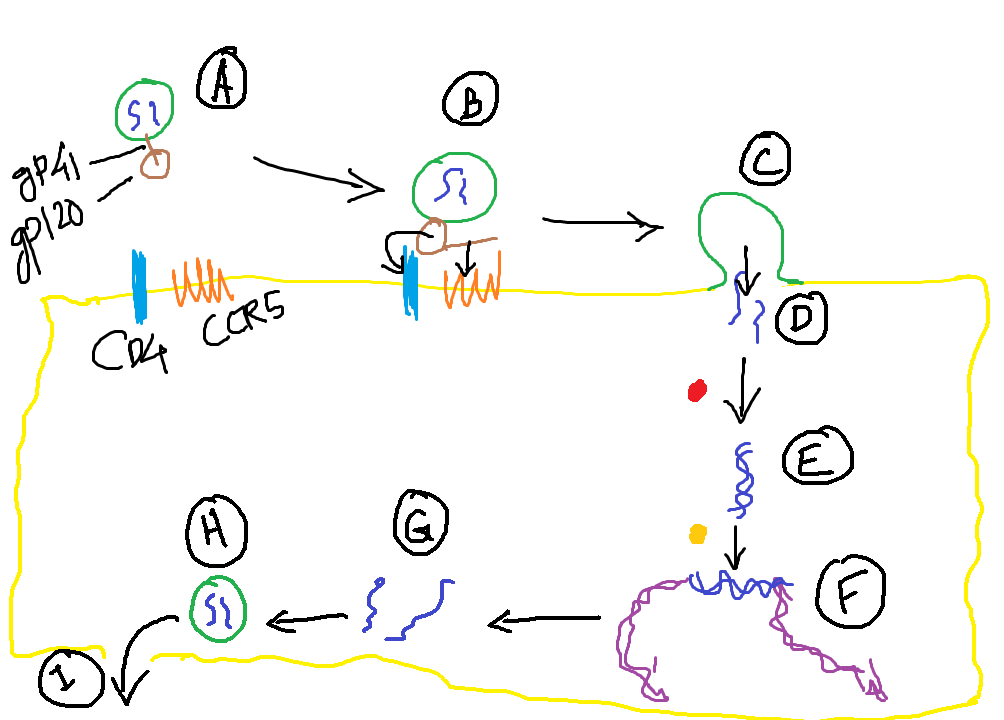
- Infection of Cells
- HIV uses CD4 molecule as a receptor and CCR5/CXCR4 (Chemokine receptors) as coreceptors (A)
- gp120 binds to CD4 → Conformational change (B) → gp120 binds CCR5/CXCR4 → gp41 facilitates fusion with host cell membrane (C) and HIV RNA enters the host cell (D)
- Viral Replication
- Reverse transcription: Viral RNA → Proviral DNA (E)
- In quiescent T cells, proviral DNA remains inactive
- In activated T cells, proviral DNA integrates into the host genome (F) → Transcription → Viral proteins (G) → Viral particles (H)
- Latent Infection
- Provirus can remain dormant for months or years
- T Cell Activation and Viral Production
- Activation by antigens or cytokines → NF-kB transcription factor → HIV gene expression → Virion production → Cell death → release of mature virion (I)
- Vicious Cycle
- HIV increases immune activation → More cytokines → More HIV production → More CD4+ T cell loss → Increased infections
Pathogenesis of HIV
Infection of Mucosal Tissues by HIV
⬇️
CD4+ T Cells & Dendritic Cells get infected by HIV
⬇️
Spread to Lymphoid Tissues (Lymph Nodes)
⬇️
Viral Replication in these Lymphoid Tissues
⬇️
Viremia (Virus in Blood)
⬇️
Widespread seeding of virus in various Lymphoid Tissues like lymph nodes, spleen, bone marrow etc.
⬇️
Host Immune Response (CTL & Antibodies) → Partial Control of Virus
⬇️
Clinical Latency Phase
Virus concentrated in lymphoid tissues
Low-level continuous viral replication
Gradual CD4+ T cell depletion
⬇️
Patient gets other infections and cytokine production
⬇️
Increased Viral Replication
⬇️
Destruction of Lymphoid Tissues → further CD4+ T cell depletion
⬇️
Severe Immunodeficiency + Opportunistic Infections → AIDS
Mechanism of Immune Depletion in HIV Infection
HIV infection of CD4+ T Cells
- Initially, the immune system compensates by producing new T cells, but over time, regeneration fails to keep up with the loss.
Mechanisms of T Cell Death:
- Direct viral killing due to: Main cause
- Membrane damage from viral budding.
- Protein synthesis defects caused by viral proteins.
- Indirect mechanisms:
- Chronic immune activation → Apoptosis of uninfected T cells (The immune system gets so hyperactive that it starts killing uninfected T cells by mistake through apoptosis).
- Disruption of lymphoid organs like spleen and lymph nodes.
- Syncytia formation (giant cells): Fusion of infected and uninfected T cells, leading to rapid cell death.
- Functional defects in surviving T cells:
- Poor antigen response.
- Shift from Th1 (cell-mediated) to Th2 (antibody-mediated) responses. (HIV reprograms the immune system — shifting the balance from virus-killing Th1 response to antibody-producing Th2 response which is HIV reprograms the immune system — shifting the balance from virus-killing Th1 response to antibody-producing Th2 response which is useless against HIV as its an intracellular pathogen!)
- Early loss of memory CD4+ T cells in mucosal tissues.
HIV Infection of Other Immune Cells
- Macrophages:
- Infected mainly by phagocytosis (Macrophages engulf HIV particles coated with antibodies or complement proteins. Once inside, instead of destroying the virus, the virus escapes into the cytoplasm. Macrophages have CD4 receptors + CCR5 coreceptors → HIV binds to them → Virus enters → Infection starts…like the Trojan horse trick!)
- Act as reservoirs, especially in late stages
- Resistant to cytopathic effects
- Dendritic Cells:
- Capture HIV at mucosal sites → Transport to lymph nodes → Transfer virus to CD4+ T cells
- Follicular dendritic cells (FDCs) bind antibody-coated virus and act as reservoirs
- B Cells:
- Not infected by HIV
- Show hyperactivation, hypergammaglobulinemia, and defective antibody responses
Latency & Reservoirs
- HIV integrates into host DNA and remains latent in memory T cells and macrophages for months or years.
- Latently infected cells act as persistent viral reservoirs, making HIV eradication difficult.
Pathogenesis of Central Nervous System Involvement
- HIV enters CNS through infected monocytes (monocytes cross the blood-brain barrier)
- Neurons are not infected
- Neurologic damage caused by viral products and cytokines from infected macrophages
Natural Course of HIV Infection
1. Acute Phase (Primary Infection)
- Occurs within 3-6 weeks after exposure
- Site of entry: Mucosal tissues → infection of memory CD4+ T cells & Dendritic Cells (DCs)
- Spread via DCs to lymph nodes → viral replication → viremia
- Symptoms:
- Acute HIV syndrome: fever, sore throat, myalgia, weight loss, lymphadenopathy, rash, diarrhea
- Spontaneous resolution in 2-4 weeks
- Seroconversion: HIV antibodies appear in 3-7 weeks
- Immune response:
- CD8+ T cells → initial containment of virus
- Viremia declines by 12 weeks but virus is not eliminated
2. Chronic Phase (Clinical Latency)
- Persistent HIV replication in lymph nodes & spleen
- Asymptomatic or mild symptoms (lymphadenopathy)
- Continuous CD4+ T cell destruction in lymphoid tissues
- Gradual decline of CD4+ T cell count
- Duration: 7-10 years (without treatment)
3. AIDS Phase
- Breakdown of immune defenses
- Dramatic rise in viremia
- Severe clinical manifestations:
- Persistent fever, weight loss, fatigue, chronic diarrhea (>1 month)
- Opportunistic infections
- AIDS-defining illnesses (e.g., Pneumocystis pneumonia, Kaposi sarcoma, CMV infections)
- Neurological diseases
Special Categories
| Category | Description |
|---|---|
| Rapid Progressors | Develop AIDS in 2-3 years (they have weaker immune response, and progress very fast to AIDS) |
| Long-Term Nonprogressors | HIV+ve for >10 years without symptoms, stable CD4+ count |
| Elite Controllers | HIV+ve with undetectable viral load (<50 copies/mL) without treatment (due to strong immune responses) |
Clinical Features of AIDS
- If no treatment is given most patients present with fever, weight loss, diarrhea, generalized lymphadenopathy, opportunistic infections, neurologic disease, and secondary neoplasms.
- Anemia, neutropenia, thrombocytopenia are common.
Opportunistic Infections:
- Pneumocystis jirovecii pneumonia: Most Common Opportunistic infection.
- Candidiasis: Most common fungal infection; oral candidiasis signals transition to AIDS.
- Cytomegalovirus (CMV): Causes retinitis (CD4+ < 50 cells/µL) and gastrointestinal ulcers.
- Mycobacterium tuberculosis & atypical mycobacteria: Disseminated infections in severe immunosuppression.
- Cryptococcosis: Meningitis in 10% of AIDS patients.
- Toxoplasma gondii: Encephalitis.
- JC virus: Progressive multifocal leukoencephalopathy.
- Herpes simplex virus: Mucocutaneous ulcers.
- Cryptosporidium hominis & enteric bacteria: Persistent diarrhea.
Tumors
- Kaposi Sarcoma (KS): AIDS-defining malignancy caused by KSHV (HHV-8).
- KS is more aggressive in AIDS patients.
- Involves skin, mucous membranes, GI tract, lymph nodes, and lungs.
- Lymphomas:
- Associated with EBV and KSHV.
- Occur in extranodal sites (CNS, GI tract, lungs).
- Primary effusion lymphoma (co-infection of EBV and KSHV).
- Burkitt lymphoma and diffuse large B-cell lymphoma.
- Hodgkin lymphoma (EBV-related).
- Cervical and Anal Cancer: Due to HPV infection.
CNS Disease
- HIV-associated neurocognitive disorder (HAND): Progressive encephalopathy.
- Peripheral neuropathy.
- (they have weaker immune response, and progress very fast to AIDS)
- Aseptic meningitis.
- Viral meningoencephalitis.
AIDS-Defining Illnesses or AIDS Indicator Diseases (CDC Criteria)
The following infections, tumors, and other conditions confirm progression to AIDS in an HIV-positive patient:
- Opportunistic Infections:
- Pneumocystis jirovecii pneumonia
- Candidiasis (Esophageal, Tracheal, or Bronchial)
- CMV retinitis
- Toxoplasma encephalitis
- Cryptococcal meningitis
- Cryptosporidiosis (chronic diarrhea >1 month)
- Mycobacterium tuberculosis (Extrapulmonary or Pulmonary if CD4+ < 200)
- Disseminated atypical mycobacterial infections (MAC)
- Progressive multifocal leukoencephalopathy (JC virus)
- Tumors:
- Kaposi Sarcoma
- Primary CNS Lymphoma
- Non-Hodgkin Lymphoma
- Invasive Cervical Cancer
- Anal Cancer
- Other Conditions:
- HIV Wasting Syndrome (Weight loss >10% + chronic diarrhea or fever >1 month)
- HIV-associated neurocognitive disorder (HAND)
Morphology of HIV/AIDS
- Lymph Nodes (Early Stage):
- Follicular hyperplasia
- Germinal center enlargement
- Lymph Nodes (Late Stage):
- Follicular involution
- Lymphoid depletion
Laboratory Diagnosis of HIV/AIDS
1. Screening Tests:
- ELISA (Enzyme-Linked Immunosorbent Assay):
- Detects antibodies against HIV viral proteins (Anti-gp120, Anti-p24).
- Most sensitive and widely used screening test.
- If positive, the test must be confirmed by a more specific test.
2. Confirmatory Test:
- Western Blot:
- Detects specific antibodies against HIV proteins (gp120, gp41, p24).
- Most specific and confirmatory test for HIV infection.
3. Direct Detection of Virus:
- p24 Antigen Capture Assay: Detects HIV core protein (p24) in blood during early infection.
- Reverse Transcriptase PCR (RT-PCR): Detects HIV RNA and estimates viral load.
- DNA-PCR: Detects proviral DNA integrated into host cells.
- Virus Culture: Isolation of HIV from monocytes or CD4+ T cells (rarely done).
4. CD4+ T-Cell Count:
- Normal count: 500–1500 cells/µL
- AIDS Diagnosis: CD4+ count < 200 cells/µL
- Used to assess disease progression and treatment response.
Treatment
- Highly Active Antiretroviral Therapy (HAART)
- Prophylaxis Against Opportunistic Infections
- Treatment of Opportunistic Infections and malignancies
Prognosis
- With early diagnosis and ART, life expectancy can be near normal.
- Without treatment, AIDS progresses in 8-10 years and leads to death within 2-3 years.
